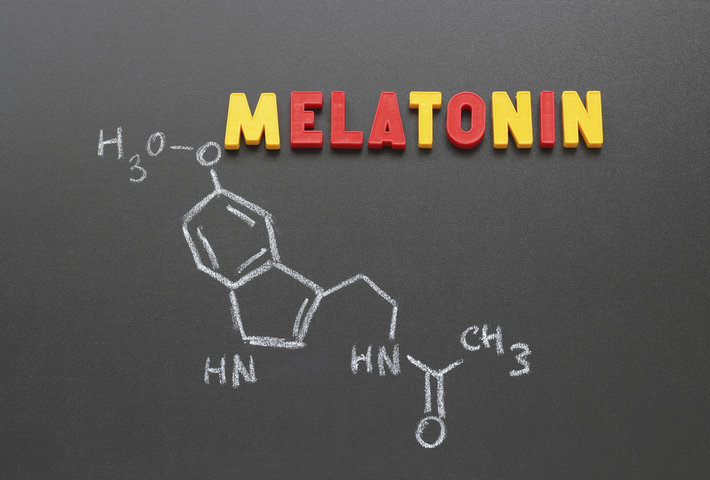
With increasing age, two diseases become more and more prominent for many women: type 2 diabetes and osteoporosis. Both often develop gradually, go unnoticed for a long time and are usually only diagnosed once the consequential damage has already occurred. The risk increases significantly after the menopause in particular. For a long time, these two clinical pictures were considered separately – but it is now becoming increasingly clear that they are more closely linked than previously assumed. A recent study has drawn attention to a rather unexpected factor: the hormone melatonin.
More than Just a Sleep Hormone
Melatonin is known to most people primarily as the “sleep hormone”. It is mainly produced at night in the pineal gland and controls our day-night rhythm. When it gets dark, the melatonin level rises and signals to the body that it is time to sleep. Light – especially blue light from screens – can inhibit this production and shift the natural rhythm. However, melatonin fulfills far more tasks in the body than just regulating sleep. It acts as a powerful antioxidant and helps to protect cells from damage caused by free radicals. This protective function is particularly important as oxidative stress plays a central role in ageing processes and chronic diseases such as diabetes and osteoporosis.
Melatonin also influences the immune system and inflammatory processes in the body. It can have an anti-inflammatory effect and helps to maintain the balance of the immune system. The hormone also has an important function in the metabolism: it interacts closely with insulin and can influence both insulin release and insulin sensitivity. A disturbed melatonin rhythm is therefore increasingly associated with the development of metabolic diseases.
Its role in bone metabolism is particularly exciting. Studies suggest that melatonin has a direct effect on the activity of bone cells. It can stimulate the so-called osteoblasts, which are responsible for bone formation, and at the same time inhibit the activity of osteoclasts, which break down bone. In this way, it helps to stabilize the balance between bone formation and bone resorption.
In addition, the body’s own melatonin production naturally decreases with age. This decline can be particularly pronounced in postmenopausal women, as hormonal changes also influence the sleep-wake rhythm. This creates a situation in which several risk factors come together: less melatonin, altered metabolic processes and accelerated bone loss.
Significantly Lower Melatonin Levels in at-risk Groups
This is precisely where the study comes in. It investigated whether there is a connection between the melatonin level in the blood and bone mineral density in postmenopausal women – and what role type 2 diabetes plays in this. A total of 190 women took part, who were divided into different groups depending on their state of health: Women with normal bone mass, women with reduced bone mass, women with diabetes and women who had a combination of both risk factors.
The results paint a remarkably clear picture. Women with diabetes or reduced bone mass had significantly lower melatonin levels than healthy participants. This difference was most pronounced in the women who had both type 2 diabetes and reduced bone density. This group had the lowest melatonin levels of all. This finding alone suggests that there is a link between hormone balance and bone health.
Link Between Melatonin and Bone Density
It gets even more interesting when you look at the relationship between melatonin and actual bone mineral density. The study shows that higher melatonin levels are associated with higher bone density. This correlation was demonstrated in both the lumbar spine and the femoral neck – two regions of the body that are particularly relevant in osteoporosis, as fractures occur here particularly frequently and often have serious consequences.
It is remarkable that this correlation was not only statistically significant, but also appears biologically plausible. Bone mineral density is the result of a dynamic balance between bone formation and bone resorption. This balance is controlled by various hormonal and cellular processes – and this is precisely where melatonin appears to intervene. It influences the activity of bone-forming osteoblasts and bone-degrading osteoclasts and thus contributes directly to the stability of the skeleton.
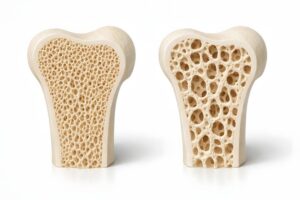
Another important aspect is that the bone density was measured in different regions of the body. The lumbar spine consists mainly of trabecular bone, which is particularly metabolically active and reacts more quickly to hormonal changes. The femoral neck, on the other hand, contains more cortical bone, which is denser and mechanically more resilient, but remodels more slowly. The correlation between melatonin and bone density in both areas indicates that the hormone has a broad influence on different types of bone. Furthermore, the consistency of the results suggests that this is not a random observation, but a systematic relationship. Low melatonin levels were repeatedly associated with reduced bone density, suggesting that a lack of this hormone could contribute to the deterioration of bone structure in the long term.
The question of temporal dynamics is also interesting in this context. As melatonin is mainly released at night, a disturbed sleep-wake rhythm – for example due to lack of sleep, shift work or exposure to light at night – could indirectly influence bone metabolism. Initial indications from other studies suggest that chronically reduced melatonin levels over longer periods of time could actually be associated with an increased risk of bone weakness.
The Role of Type 2 Diabetes
However, melatonin does not appear to act independently of other factors. Type 2 diabetes plays an important role in how strongly the hormone affects the bones. This became particularly clear in the area of the femoral neck. There it was shown that diabetes “mediates” a considerable part of the effect. Put simply, this means that a disturbed sugar metabolism can partially weaken the protective effect of melatonin on the bones. Interestingly, this effect was not observed in the same way in the lumbar spine, which indicates that bones in the body react differently to hormonal and metabolic influences.
In addition to these correlations, the study also provides evidence that melatonin could possibly be used as a diagnostic marker. The statistical analysis showed a surprisingly high degree of accuracy in differentiating between healthy women and those with reduced bone mass. The high specificity was particularly striking: low melatonin levels were indeed associated with a very high probability of impaired bone health. This opens up the prospect that simple blood tests could help to identify at-risk patients earlier in the future.
Why Postmenopausal Women are Particularly Affected
But why are postmenopausal women in particular so badly affected? The answer lies in a complex interplay of hormonal changes. With the onset of the menopause, oestrogen levels drop significantly. Oestrogen normally protects the bones by inhibiting their breakdown. If this protection is lost, the bone substance is reduced more quickly. At the same time, the sleep rhythm changes in many women, which in turn can affect melatonin production. In addition, the risk of insulin resistance and therefore type 2 diabetes increases. These factors reinforce each other and together can have a negative impact on bone metabolism.

At a biological level, there are several possible explanations as to why melatonin plays such an important role. On the one hand, it appears to have a direct effect on bone cells by promoting their formation and inhibiting their breakdown. Secondly, it protects the cells from oxidative stress, which plays an important role in both diabetes and osteoporosis. In addition, melatonin influences sugar metabolism, meaning that low levels may also indirectly damage bones by worsening diabetes.
The results of the study therefore also have practical significance. They suggest that bone health should not be considered in isolation. Factors such as sleep quality, hormonal balance and metabolism are interrelated and should be considered together. For medical practice, this could mean that in future, melatonin levels will also be looked at more closely in women with an increased risk of osteoporosis.
Can Melatonin be Used Therapeutically?
The question of whether melatonin itself can be used specifically as a therapy to support bone health is becoming increasingly important. While there is not yet enough data to derive clear guideline recommendations, there is growing evidence that melatonin could be a promising approach – especially in postmenopausal women with an increased risk of osteoporosis.
A key advantage of melatonin is its broad action profile. It intervenes simultaneously at several points in processes that are crucial for bone metabolism. Experimental and initial clinical studies show that melatonin can promote the activity of osteoblasts, the cells responsible for bone formation. At the same time, it appears to inhibit the activity of osteoclasts, which break down bone tissue. This dual effect is particularly interesting, as many existing therapies tend to either inhibit bone resorption or promote bone formation. In addition, melatonin has an antioxidant and anti-inflammatory effect – two properties that play an important role in chronic diseases such as type 2 diabetes. As oxidative stress and chronic inflammatory processes can accelerate bone loss, melatonin could have an indirect stabilizing effect on bone substance. In this context, it is also being discussed whether melatonin can help to at least partially mitigate diabetes-related bone damage.
Another potential benefit is the improvement in sleep quality. Sleep disorders are common in postmenopausal women and are themselves linked to hormonal imbalances and metabolic problems. By stabilizing the sleep-wake rhythm, melatonin could therefore contribute not only directly but also indirectly to bone health. Regular, restful sleep supports numerous regeneration processes in the body – including bone metabolism.
Initial small-scale studies and experimental investigations have already provided indications that melatonin supplementation could have a positive effect on bone mineral density. Especially in combination with other measures – such as sufficient calcium and vitamin D intake or physical activity – a synergistic effect could result. This makes melatonin an interesting component of a holistic prevention or therapy concept.
Conclusion
The current findings clearly indicate that melatonin plays a much greater role in bone health than has long been assumed. Particularly in postmenopausal women – and even more so if they also have type 2 diabetes – a low melatonin level could be a decisive, previously underestimated risk factor for the loss of bone mass.
Against this background, melatonin appears to be a promising approach that influences several relevant processes at the same time: it supports bone formation, counteracts bone loss and also has antioxidant and metabolism-regulating effects. This combination makes it particularly interesting for a holistic approach to the prevention of osteoporosis.
Even if further studies are needed to define the dosage and long-term effects more precisely, the results so far speak for themselves. Melatonin has the potential to establish itself as a useful component of modern prevention strategies – especially in a phase of life in which hormonal changes and metabolic processes are closely linked. This means that melatonin is increasingly coming into focus not only as a sleep hormone, but also as a versatile health regulator that can also play an important role in the stability of our bones.