Back pain is one of the most common health problems worldwide; it affects people of all ages and places a considerable burden on healthcare systems. Lower back pain in particular is widespread. For many patients, the pain becomes chronic and interferes with work, sleep and everyday life. In most cases, however, doctors are unable to identify a clear structural cause, making effective long-term treatment difficult. Research suggests that a widely used bone hormone could help relieve chronic back pain in unexpected ways. Rather than simply strengthening the bones, it appears to prevent pain-sensitive nerves from growing into damaged areas of the spine. In animal models, this led to a strengthening of the spinal tissue and reduced sensitivity to pain. The results point to a future treatment method that combats back pain at its biological cause.
A new study published in Volume 14 of the journal Bone Research shows that a hormone-based treatment could help relieve chronic back pain by reducing abnormal nerve growth in damaged spinal tissue. The research was led by Dr. Janet L. Crane of the Center for Musculoskeletal Research, Department of Orthopaedic Surgery, at Johns Hopkins University School of Medicine in the United States. The results offer new insights into how bone cells can influence pain signaling in degenerating spines. “When the spine degenerates, pain-sensitive nerves grow into areas where they are not normally found. Our results show that parathyroid hormone can reverse this process by activating natural signals that push back these nerves,” said Dr. Crane.
How Back Pain is Treated
There is a whole range of treatment approaches available today for back pain – especially the common low back pain. Which therapy is appropriate depends largely on the cause, the duration (acute vs. chronic) and the severity of the symptoms. In practice, several methods are often combined. One of the most important pillars is exercise and physiotherapy. Targeted exercises strengthen the back muscles, improve mobility and stabilize the spine. Methods such as manual therapy or back training are also often used to correct incorrect posture and make everyday life easier on the back.
Medication is often used as a supplement, especially to relieve pain. These include classic painkillers such as ibuprofen or paracetamol. For more severe symptoms, muscle relaxants or – in selected cases – stronger painkillers may also be prescribed in the short term. The main aim here is to maintain mobility, as relieving posture often exacerbates the symptoms. Another important area is minimally invasive procedures. These include injections in which anti-inflammatory medication is injected directly into the painful area, for example at nerve roots or in facet joints of the spine. Such procedures can be particularly helpful in cases of inflammatory or nerve-related pain.
If conservative measures are not sufficient and there is a clear structural cause – such as a herniated disc or a pronounced narrowing of the spinal canal – surgery can also be considered. The aim is then to relieve pressure on the nerves or restore stability to the spine. However, surgery is usually only performed once other therapies have been exhausted. In addition to these physical approaches, the psychosocial component also plays a major role, especially in cases of chronic pain. Methods such as cognitive behavioral therapy help to improve the way we deal with pain and break so-called pain cycles. Newer and experimental approaches – such as treatment with parathyroid hormone – aim to intervene more deeply in the biological causes.
The Parathyroid Hormone and its Effects
Parathyroid hormone (PTH) is produced naturally by the parathyroid glands and plays a key role in regulating calcium levels and bone remodeling. Its central task is to finely regulate the calcium level in the blood, as calcium is essential for many basic bodily functions, such as muscle contraction, signal transmission between nerve cells and bone stability.
When the calcium level in the blood drops, parathyroid hormone is released. It then acts on several organs simultaneously: in the bones, it stimulates the breakdown of bone substance, releasing calcium. In the kidneys, it ensures that less calcium is lost via the urine and more phosphate is excreted at the same time. PTH also indirectly stimulates the formation of active vitamin D, which increases the absorption of calcium from food in the intestine. This coordinated interaction raises the calcium level in the blood back to a normal level.

Interestingly, parathyroid hormone has different effects on the bones depending on how it is released. While a permanently elevated PTH level – for example in certain diseases – can lead to bone weakness, a short-term, controlled administration of synthetic PTH has exactly the opposite effect: it promotes bone formation. Synthetic versions of PTH are already being used to treat osteoporosis. Previous research suggested that these treatments could also alleviate bone-related pain, but the underlying biological mechanism was not yet well understood.
To investigate this further, the research team used three mouse models that mimic common causes of spinal degeneration: natural aging, surgically induced mechanical instability and genetic susceptibility. These models allowed the scientists to study how degeneration affects both bone structure and nerve growth. The mice received daily injections of PTH over a period of two weeks to two months, while the control animals were given inactive solutions. The researchers then examined the spinal tissue using high-resolution imaging and measured the reactions to pressure, heat and movement.
Improved Spinal Structure and Reduced Pain Sensitivity
After one to two months of treatment, the mice treated with PTH showed significant improvements in their vertebral endplates, the thin layers that separate the intervertebral discs from the vertebrae. These structures became denser and more stable. At the same time, the treated mice showed reduced sensitivity to pain, tolerated pressure better, reacted more slowly to heat and showed increased activity compared to untreated animals.
The researchers also examined the nerve fibers within the spinal column. In damaged tissue, pain-sensitive nerves often spread to areas where they do not normally occur, which increases the discomfort. The study found that PTH treatment significantly reduced these abnormal nerve fibers using markers such as PGP9.5 and CGRP. Further analysis revealed the underlying mechanism. PTH stimulated osteoblasts, the cells responsible for bone formation, to produce a protein called Slit3. In simple terms, Slit3 can be thought of as a biological orientation signal: It tells growing nerve fibers where to grow – or where not to grow. This protein acts as a guiding signal that fends off growing nerve fibers and prevents them from penetrating into sensitive areas of the spinal column.
Laboratory tests have confirmed that Slit3 directly inhibits nerve growth. When nerve cells were exposed to Slit3, their sprouts became shorter and less invasive. In contrast, when the researchers removed Slit3 from mouse osteoblasts, PTH no longer reduced nerve growth and did not improve pain responses. The team also identified a regulatory protein called FoxA2 that helps trigger Slit3 production in response to PTH, providing deeper insights into how hormonal signals influence nerve behavior.
What this Means for Future Back Pain Treatments
Although these findings come from animal studies, they may help explain why some patients receiving PTH-based treatments for osteoporosis report reduced back pain. The researchers point out that further studies in humans are needed before this approach can be applied clinically. “Our study suggests that PTH treatment of LBP in spinal degeneration may reduce abnormal innervation, setting the stage for future clinical trials investigating the efficacy of PTH as a disease-modifying and pain-relieving treatment in spinal degeneration,” Dr. Crane said.
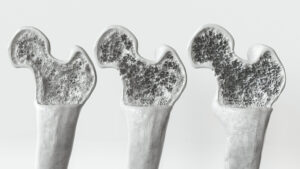
If PTH – mediated via osteoblasts and the protein Slit3 – inhibits precisely this uncontrolled nerve growth, the therapy would not only dampen symptoms, but also directly address one of the causes. This makes the approach particularly promising: it combines structural regeneration (more stable vertebral endplates, improved bone quality) with a biological “reorganization” of the pain conduction pathways. In practice, this could mean that patients not only feel less pain, but are also less susceptible to chronic courses in the long term.
PTH works differently depending on how it is administered: short-term, controlled doses promote bone formation, while permanently elevated levels can even be harmful. For use in back pain, however, it would still have to be precisely defined how often and in what dose the hormone is administered in order to achieve the desired effect on bones and nerves without risking side effects. There is also the question of which patient groups would benefit the most. The most likely benefit is in people with clearly demonstrable spinal degeneration, such as disc wear or changes in the vertebral end plates. The approach could be less suitable for non-specific back pain without a recognizable structural cause. Another exciting aspect is the identification of the regulatory factor FoxA2. This protein mediates the effect of PTH on the production of Slit3. In the long term, this could lead to even more targeted therapies, for example by intervening directly in this signaling pathway without affecting the entire hormone system.


