Stiff knees, aching hips and persistent joint pain are often dismissed as normal signs of ageing. But osteoarthritis, the world’s most common joint disease, is not being treated according to actual research findings. Experts say that the biggest problem is not the lack of treatment options, but that the most effective method is not being used.
Why Exercise Protects the Joints
The most effective treatment is not found in a medicine bottle or in the operating room. It is physical activity. It is widely regarded as one of the best treatments for long-term joint conditions such as osteoarthritis. Yet it is only prescribed to a minority of patients. Studies from Ireland, the United Kingdom, Norway and the United States show a consistent pattern. Less than half of people diagnosed with osteoarthritis are referred to exercise programs or physiotherapy by their GP. More than 60 percent receive treatments that are not recommended in clinical guidelines, and about 40 percent are referred to a surgeon before non-surgical options have been adequately explored.

To understand why this is important, it helps to look at how joints actually work. Osteoarthritis is the most common form of arthritis and already affects more than 595 million people worldwide. An extensive analysis published in The Lancet comprehensive analysis estimates that the number of people living with osteoarthritis could rise to one billion by 2050. Longer life expectancy, increasingly sedentary lifestyles and rising rates of overweight and obesity are contributing to this increase. Regular physical activity not only alleviates symptoms. It can biologically and physically lower the risk of developing osteoarthritis and reduce its severity.
Cartilage, the smooth tissue that cushions the ends of bones, has no blood supply of its own. It relies on movement to stay healthy. When you walk or put weight on a joint, the cartilage is gently squeezed, forcing fluid out. When the pressure is released, it soaks up the fluid again, bringing nutrients and natural lubricants with it. Each step helps to nourish and maintain the joint. For this reason, it is misleading to refer to osteoarthritis simply as “wear and tear”. Joints are not like tires that inevitably break down over time. Instead, osteoarthritis is better understood as a long process of degradation and repair. Regular exercise plays a key role in supporting healing and maintaining the health of the joint as a whole.
Osteoarthritis is a Disease of the Entire Joint
Osteoarthritis does not only affect the cartilage. It affects the entire joint, including joint fluid, underlying bones, ligaments, surrounding muscles and even the nerves that control movement. Targeted exercises address many of these components simultaneously. Muscle weakness is one of the earliest warning signs of osteoarthritis, and strength training can help reverse it. There is strong evidence that weak muscles increase both the risk of developing osteoarthritis and of the disease progressing more rapidly.
Neuromuscular training programs such as GLA:D® (Good Life with osteoArthritis: Denmark) have been developed specifically for people with hip and knee osteoarthritis. These programs are usually offered in supervised group sessions under the guidance of physiotherapists and focus on improving movement quality, balance and strength. The aim is to improve joint stability and restore confidence in movement. Participants in these programs report significant pain relief, better joint function and improved quality of life that lasts up to 12 months after completing the program.
Exercise has a positive effect on the whole body. It has proven benefits for more than 26 chronic diseases. In osteoarthritis, its effects go beyond strengthening the muscles and supporting the cartilage. It also combats inflammation, metabolic changes and hormonal shifts that contribute to the disease.
Inflammation, Obesity and Joint Damage
Obesity is a major risk factor for osteoarthritis, and the reason for this is not just the extra stress on the joints. Excessive body fat is linked to higher levels of inflammatory molecules in the bloodstream and joint tissue. These substances can damage the cartilage and accelerate the progression of the disease. Regular physical activity helps to counteract these effects at the molecular level counteract. It can lower inflammatory markers, reduce cell damage and even influence gene expression in a way that supports joint health. In recent years, it has been shown that metabolic and inflammatory mechanisms also play a central role. Adipose tissue is not just a passive energy store, but a hormonally active organ that produces numerous biologically active molecules. These include so-called adipokines and pro-inflammatory cytokines, which can contribute to the development of a chronic low-grade inflammatory state in the body.

Exercise Before Surgery
There are currently no medications that can alter the basic course of osteoarthritis. Joint replacement surgery can make a big difference for some people, but it is a major procedure that does not work equally well for everyone. Commonly used agents include non-steroidal anti-inflammatory drugs, which have an anti-inflammatory and pain-relieving effect. Although these drugs can improve the quality of life of many sufferers, they do not directly intervene in the underlying degenerative processes of cartilage degradation. For this reason, intensive research is being carried out into so-called disease-modifying therapies that could intervene specifically in the biological mechanisms of osteoarthritis in the future.
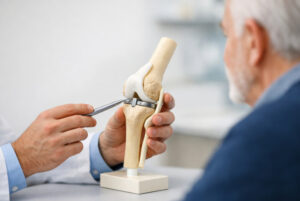
If conservative measures such as exercise therapy, weight reduction, physiotherapy and pain medication are no longer sufficient, surgical treatment can be considered in advanced stages of the disease. A common option is the use of an artificial joint, such as a knee or hip endoprosthesis. In this surgical procedure, severely damaged joint surfaces are removed and replaced with artificial implants that are designed to replicate the function of the joint as closely as possible. For many patients, such an operation can mean a significant improvement in quality of life, as pain is reduced and the joint’s mobility and load-bearing capacity can be restored. Despite these potential benefits, however, it is a major surgical procedure that is associated with certain risks. These include infections, complications during or after the operation and possible loosening or wear and tear of the implant over time. In addition, the recovery process varies from person to person and usually requires a longer phase of rehabilitation and physiotherapy in order to train the joint to function optimally again. In addition, not all patients benefit to the same extent from a joint replacement. Factors such as age, general state of health, muscle strength, body weight and the extent of joint damage can influence the success of the operation. For this reason, the decision to have a joint replacement is usually carefully considered on an individual basis and only made when other treatment options are no longer sufficiently effective.
Exercise should be the first step and remain part of the treatment at every stage of the disease. It carries far fewer risks than surgery and has far-reaching health benefits beyond the joints. Osteoarthritis is not just about “worn out” joints. It is influenced by muscle strength, inflammation, metabolism and lifestyle factors. Regular, structured exercise affects many of these factors simultaneously, helping to protect cartilage, support the entire joint and improve overall health. Before opting for surgery, exercise remains one of the most effective treatments.